Introduction
The heart is one of the most fascinating organs of the human body. It is a superb mechanism, manifesting great wisdom in its construction. It is the central organ of the circulatory system' acting as a force and suction pump in relation to the blood vessels. Excepting the lungs, it is the only organ in the body through which the blood passes in every cycle. Activity of the heart is necessary to life. The average human heart, beating at 72 beats per minute, will beat approximately 2.5 billion times during a lifetime (about 66 years).
Heart disease is one of the biggest killers in the world. During the last few decades, heart failure has developed into a major burden in the Western world, increasingly affecting millions, who suffer a poor quality of life, characterised by debilitating symptoms, frequent hospitalisation and a poor quality of life. Also, current figures in the UK indicate that heart failure is a major public health problem nearing epidemic proportions; approximately 250,000 new cases of various heart failure stages are diagnosed each year (www.bhf.com). For these reasons, research into the causes and consequences of heart disease has key importance in order to improve the current strategies for its prevention and treatment in primary and secondary care.
Myocardial infarction (MI) is a leading cause of premature morbidity and mortality. Acute MI causes death of heart muscle tissue, scar formation in the area of infarction, border zone abnormalities, and compensatory hypertrophy in areas of the heart remote to the MI. Collectively, these pathologies result in reduced pump function, adverse remodelling and heart failure.
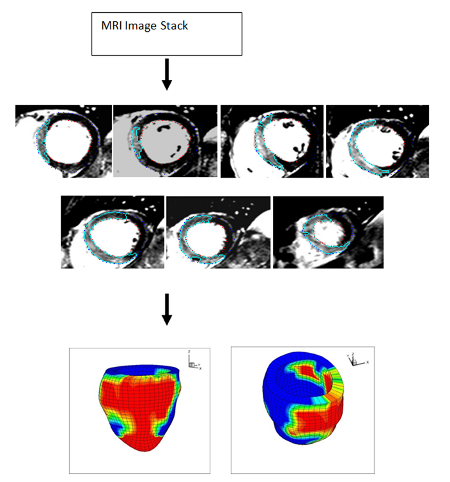
Figure 1, from in-vivo cardiovascualr magnetic resonance images to a computational left ventricular model with delineated oedema regions.
Imaging the heart provides information on heart structure and function and cardiac magnetic resonance imaging (MRI) is the gold standard. Imaging is a cornerstone of risk assessment and, for example, cardiac imaging quantifies left ventricular ejection fraction which is essential to inform evidence-based drug treatment. In fact, heart imaging, and cardiac MRI in particular, reveals much more about the heart, including structure, function, volumes and injury, all of which are linked to pathology. The strength of MRI is the in-depth information that is provided, however because of technical limitations, the information can be complex and not straightforward to use for risk assessment in routine clinical practice.
Computed modelling represents a solution to this problem. Using mathematical and computational techniques, modelling has the potential to bring together all of the information from a cardiac MRI scan into a single clinically-useful form. Indeed, heart modelling with the aim to combat diseases is at the frontier of biomechanics research. New imaging techniques and advanced modelling of a “static” heart have reached to the stage that it is now possible to develop a whole heart model with predicating power.
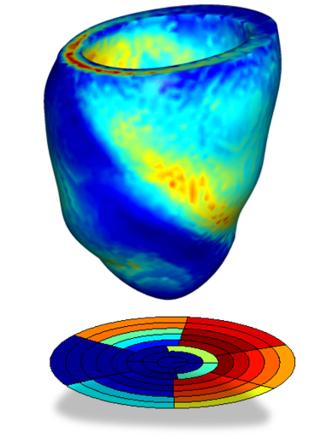
Figure 2, A computerized simulation of a human patient heart at six months later after acute myocardial infarction, which is locating in the left side of the heart. The top image is the systolic myofibre stress, the high stress region along myocardial infarction is believed to be a critical stimulus for adverse remodelling. The bottom image is the systolic active force with impaired contractility in the myocardial infarction. Blue to red represents low to high values.

